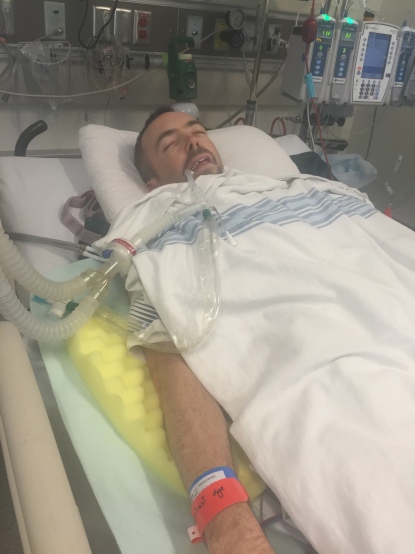
Waking up from surgery is a very surreal experience. The first notion of any kind of thought in my head was, “Wait…what….I think surgery is done and I’ve lived”. I tried to take in my surroundings while making an attempt to open my eyes. I managed one eye open and ended up with a look somewhere between disdain and surprise. I knew going in that the breathing tube may be still down my throat so my first efforts at being part of the world again surrounded me trying to get a sense of where the tube was and how to control my breathing. I tried to remain calm and could hear voices in the background of my wife and the staff in the ICU. I went in and out of consciousness for what may have been several hours until I really got tired of the breathing tube being in. At one point I woke and saw a couple of girls at the foot of my bed and I motioned to my mouth while gesturing that I’d like to have the tube removed. It happened that these girls were Respiratory Therapists there to do just that. They came over and gave me a brief that they would be taking the tube out and to try to exhale and cough as best I could. The feeling of a long tube coming out of my throat wasn’t painful. It was just very weird and caused me to gag and to make some noise resembling a long cough. The act of participating in that event made me very tired and I immediately fell asleep. Right away the nurse and my wife woke me up as I went into a “non breathing” apnea which apparently is quite common. I thought they were both being quite rude waking me up as all I wanted to do was to go to sleep.
I know from looking at the pictures, my eyeballs show that I was very much sedated but the pain level was mostly controlled. I knew as soon as I woke up that the surgery had completely done a number on me and it was going to be a much bigger deal than I had anticipated. My energy was eliminated and I felt like a very fragile bird in a nest. I went into surgery at 0730 and it was done by around 11am. The surgeon came out and told my wife that my Aortic Valve was very “Crummy” and he was surprised by what I had accomplished with my Bicuspid Valve. I can’t say enough about the surgeon and his amazing skill. Just a day at the office for him is a day which changed my life entirely.
The rest of the day went by with shift changes and medication being given. I took inventory of tubes and attachments. I had an IV in my left arm, a monitor hooked into my left wrist, a central IV line on my chest, two drainage tubes coming out of my chest, a huge dressing down my chest incision, and a catheter line coming out between my legs. I was at that time on morphine and at a pain level of about a two to three so not bad at all. The male nurse bathed me late in the day which actually was very nice to get all the iodine off and felt like a very caring and connective experience. There were interruptions through the night as people came and went from the bed beside me and hearing the family stress of a family member suddenly in ICU made me feel lucky that I had time to prepare both mentally and physically with getting ready for this surgery. I went into this in great shape and was in control of the decisions on surgery and valve selection. In emergency situations many aren’t so lucky.
I was thankful to be alive and have the support of my wife, sister and brother in law who were there for me during this time. I under-estimated how much this would affect me physically as well as emotionally. I felt miles from being who I was just a short time before.







